This article was originally published in the CTC Live 2020 Fight to Win paper.
In the history of modern warfare, combat first aid has contributed to the survivability of combatants on the battlefield. Without effective combat first aid and subsequent responsive evacuation, the risk to personnel and mission is increased. World War One (WW1) and Operation Iraqi Freedom (OIF) highlight the changes to medical support that have saved lives and increased decision superiority. Advancements in medical procedures and technologies, as well as training, tactics and procedures, improved the survivability of casualties on the battlefield, all the while enabling decision superiority by allowing commanders to focus on the tactical situation knowing casualties were being appropriately cared for.
The battlefields of WW1 bear little resemblance to modern battlefields, particularly since casualties were inflicted on a far larger scale than more recent operations. In July, 1916 during the Battle of Fromelles, the Australian Imperial Force suffered 5,533 casualties, of which almost 2,000 were killed. The development of weapon technology contributed to the large number of casualties, with artillery fire alone accounting for two thirds of all casualties on the Western Front. Armies had to develop new means and methods in the conduct of casualty treatment, care, and evacuation to cope with the increase in the scale of casualties.
Prior to WW1, porters moved casualties from the battlefield. The changing characteristics of war necessitated stretcher bearers with medical training that could provide point-of-injury treatment to the casualty. These stretcher bearers were the forebearers to the modern medical technician, and they were responsible for the application of pain relief, dressings to wounds and splints.[1] Stretcher bearers provided casualty care and evacuation under constant threat of enemy fire and with limited respite. Following the initial engagement of the Battle of Passchendaele in 1917, it took three days to clear the battlefield of casualties because stretcher bearers had to conduct a three-mile round trip to move the injured to safety.[2]
After initial treatment, casualties were transported to the regimental aid post, which was located close to the front line and vulnerable to enemy fire. From the regimental aid post, casualties were transported down the line to a casualty clearance station to be triaged and placed into three broad categories: those who required minimal care, those who required immediate care to survive, and those who were unlikely to survive regardless of treatment.
Throughout WW1, medical advancements were identified and incorporated to enhance survivability of casualties. Splints were responsible for saving the lives of 80% of casualties with broken thigh bones in 1916 who, if they had suffered the injury two years prior, would have likely died.[3] The development of effective local and general anaesthesia prior to WW1 enabled surgeons to undertake procedures previously beyond them. Debridement (the removal of dead tissue) became a standard surgical practice following the recognition of the dangerous role of bacteria in post-surgery infections. Similarly, the sterilisation of all medical equipment before reuse greatly improved the confidence of surgeons.[4] These practices enabled surgeons to improve post-surgery survival rates.
Nearly 100 years later, OIF continued advancements in the care of battlefield casualties. Prior to the introduction of Tactical Combat Casualty Care (TCCC), US medical personnel were taught to conduct battlefield trauma care with limited consideration of the tactical situation.[5] TCCC uses the Combat Applied Tourniquet, haemostatic dressings, and improvement in airway management to enable early medical intervention at the point of injury without compromising the tactical situation. When combined with a phased medical system, the TCCC achieved its aim to, 'ensure that good medicine is combined with good small-unit tactics.'[6]
During the US advance to Baghdad in 2003, tourniquets were decisive in stopping haemorrhaging in soldiers with serious extremity wounds. This allowed casualties to be kept alive until the tactical situation permitted evacuation to forward surgical treatment teams.[7] Data from one US Army shock surgical platoon deployed to Iraq reveals that of all operative patients, 94% suffered from high energy wounding.[8] During the implementation and training period from 2006 to 2007, tourniquets reduced deaths from extremity haemorrhage from a rate of 23.3 deaths per year to 17.5; after full implementation this rate was reduced to 3.5 deaths per year.[9] Of the US casualties in Iraq and Afghanistan as of 2008, well over 1,000 US soldiers’ lives were saved with tourniquets.[10]
While medical advancements saved the lives of soldiers deployed on OIF, distance continued to present challenges to the medical system. The rapid movement of combat forces during the initial invasion phase of OIF needed to be supported by a medical system that could keep pace, as medical studies recognised that for every combatant that dies, there are between four to six combatants that are severely injured.[11] US forces were able to shorten the distance and time to medical care and increase the survivability rates of casualties by using surgical shock trauma platoons forward in the battle space.[12] Despite these forward medical capabilities, soldiers still died when the time required for casualties to reach medical facilities was too great. Data from 2001 to 2011 showed that of the combat deaths in Afghanistan and Iraq, nine out of ten occurred prior to arrival at a medical facility, with 24.3% of these deaths likely preventable.[13] However, units that utilised TCCC, combined with a command-directed casualty response system, reduced preventable deaths. The US TCCC-based Ranger First Responder program utilised by the 75th Ranger Regiment was able to reduce the unit’s incidence of preventable death to the unprecedented low level of 3% of their total fatalities.[14]
WW1 and OIF highlight the importance of an effective medical system to support combatants and prevent the loss of life. In both conflicts, medical personnel were utilised to provide care to casualties at point of injury. An echelon system of medical care was used to increase the responsiveness of medical personnel and assets, which resulted in increased patient survivability. The continued use of advancements in medical procedures and technologies both at the point of injury and during subsequent treatment also enhanced the casualty's outcome.
The Australian Army, like the US Army, utilises TCCC as the means of training and preparing basic first responders in the initial care and treatment of combat causalities in a tactical environment. TCCC is one of the Army’s combat behaviours and it contributes to the effectiveness and survivability of casualties from the point of injury to definitive care, while also enabling the best care for casualties through the Land Based Trauma System. Soldiers that are proficient in combat first aid provide commanders with a force that can react decisively when faced with traumatic situations. Additionally, the issuing of individual first aid kits to all soldiers allows fast and responsive treatment at the point of injury. The introduction of tranexamic acid to prevent or treat excessive blood loss from major trauma has increased a casualty’s life expectancy prior to reaching definitive care. This increase in time gives a commander greater latitude in treating the tactical threat before having to provide personnel to support casualties, improving overall tactical decision superiority.

Modern casualty collection point scenario
The reduction of casualties from WW1 to OIF demonstrate that close and reactive medical care has a positive impact on the survivability of casualties. The Australian Army operates an echelon medical system that includes advanced first aid being conducted at the point of injury, then advanced resuscitation being undertaken by a treatment team, and finally damage control surgery undertaken at a Role 2 Enhanced or higher medical facility. This system is framed around the '10-1-2' or 'golden hour' rule for movement of a casualty to care. As seen in previous conflicts; however, delays in the movement of casualties due to the tactical situation, availability of evacuation assets, and distance to medical facilities will affect the survival rates of seriously wounded combatants. WW1 and OIF demonstrate that commanders need to consider the speed of advance and the location of medical assets to appropriately balance the tactical and medical risks.
Noting that delays in movement of casualties will cause additional deaths, it is imperative that casualty care and evacuation be given the appropriate attention in training to ensure it is undertaken to the highest standard on operations. Soldiers need to be equipped and regularly trained in TCCC. CASEVAC routes (inclusive of casualty collection points and ambulance exchange points) need to be rehearsed and detailed in orders, at all echelons, to ensure all personnel are aware of their roles and responsibilities when delivering aid to casualties. While the tactical situation dictates the movement of casualties from point of injury, commanders need to consider risk to mission success against risk to casualties. Consideration should be given to rates of advance and the placement and security of forward medical treatment teams, as this will impact on the survivability of casualties. By building a responsive medical system that does not require a shift in focus from the tactical situation to casualty care, commanders will gain decision superiority over adversaries with less advanced plans.
The current process utilised by the Australian Army to track a casualty’s location on the battlefield is done in near real time, via voice and digital reporting. The casualty’s location is relative to the last update. There is limited ability to digitally pass a casualty’s medical condition report from point of injury through to subsequent medical providers as the casualty moves rearward through the battle space. Additionally, there can be a lack of awareness between tactical formations and the Casualty Regulation Centre, as they often operate on different networks. This can lead to confusion within headquarters, delays in casualty evacuations, and impact on decision superiority as commanders focus on casualty evacuation rather than the tactical situation.
Accelerated Warfare tasks the Army to 'leverage emerging technology as a potential source of advantage.'[15] Advancements in health-state monitoring could be incorporated into a casualty regulating and command and control evacuation system. This would allow early identification of casualties to reduce response time of evacuation platforms and also provide clinicians with forewarning of casualties’ medical conditions to enhance triage and responsiveness. Through the utilisation of emerging technologies and other Defence capabilities, Army can close the gap in the current battlefield casualty tracking system. A responsive medical system will provide greater situational awareness to commanders and health planners and allow commanders to focus on the tactical situation, enhancing decision superiority.
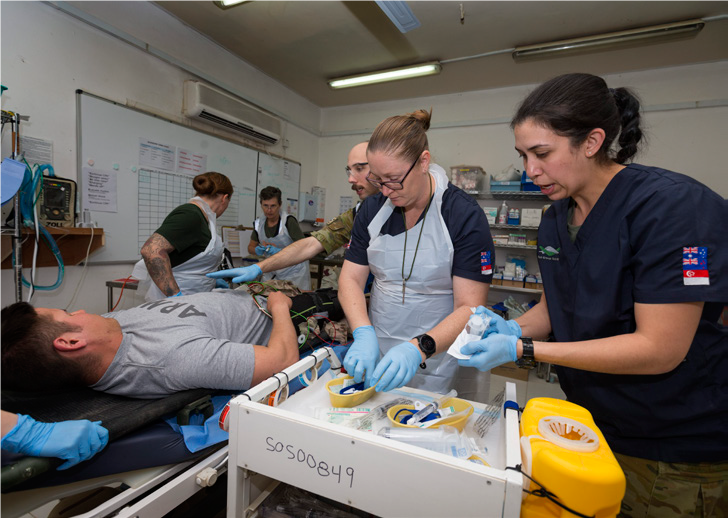
Modern war and medical treatment facilities
From WW1 to OIF, advancement in medical technologies from the splint to the combat tourniquet, training soldiers and medical personnel in the provision of first aid, and utilising a responsive, tiered medical system have enhanced the survivability of combatants on the modern battlefield. These advancements have broadened commanders’ decision superiority by allowing a commander time to deal initially with the tactical situation rather than to divert combat troops to the support of casualties. Training in TCCC, conducting comprehensive training in CASEVAC, and ensuring medical assets are tactically positioned to provide timely care to a casualty will improve the outcomes for all soldiers on the battlefield, not least lend to regaining or maintaining the initiative. The ADF should embrace emerging technologies that can digitally identify casualties, prioritise health support, and reports casualties’ medical status and location across the battlespace. It is through using the past to guide the future that the ADF will ensure that it is ready to save a life, while maintaining the fight.